We can win the battle against cancer if we discover soon enough that it has begun to grow.
The earlier suspicious lesions can be observed, the better the chance for prompt appropriate therapy and successful treatment. Unfortunately, the longer the cancer grows, the worse it gets: the abnormal cells begin to occupy neighboring tissues, can enter the bloodstream, and then circulate throughout the body with the blood (resulting in metastasis), and it becomes increasingly difficult to treat.
That is why it is so important for our health and even life to recognize the earliest signs that something wrong is happening in the body.

When to report for an NBI diagnostic test?
- Unexpected change in tone of voice: seems more dull, low.
2. Emerging difficulty when speaking – longer speech causes fatigue and the voice is weaker.
3. Persistent hoarseness that has been present for several weeks.
4. Frequent coughing, as well as scratching, burning, pinching, or stinging in the larynx (when these symptoms are not related to infection, i.e., not accompanied by fever, runny nose, etc.)
6. Prolonged or recurrent pain in the forehead, orbit, nasopharynx, larynx and ears.
7. Unilateral hearing loss.
8. Recurrent nosebleeds.
9. Coughing up blood-colored secretions.
What can cause cancer?
Causes of cancer formation and development
NBI diagnostics should be used by people at risk, meaning those who:
- Have daily contact (e.g. at work) with chemical reagents, stay in a dusty, polluted environment.
2. Smoke cigarettes (or have smoked in the past), and who are passive smokers (i.e., those who stay in the room with smokers).
3. People whose relatives (immediate family) have had upper respiratory tract cancer (e.g., laryngeal, pharyngeal, oral cancer)
Note! It is also a test recommended for anyone concerned about their health. It is a good idea to include NBI in your set of preventive screenings and have them done regularly every 12 months.
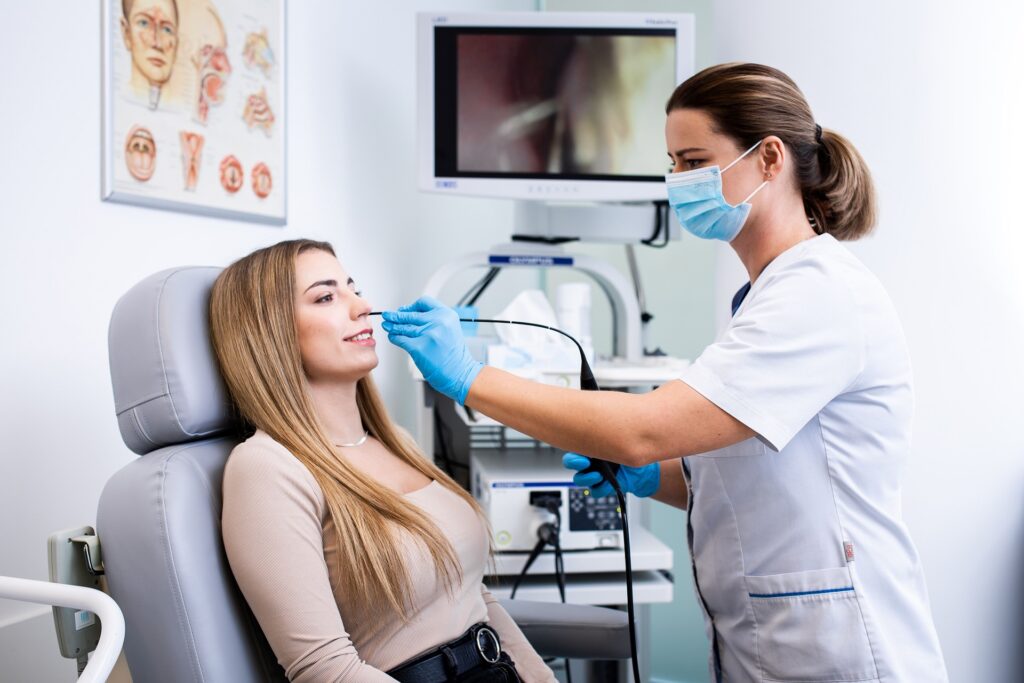
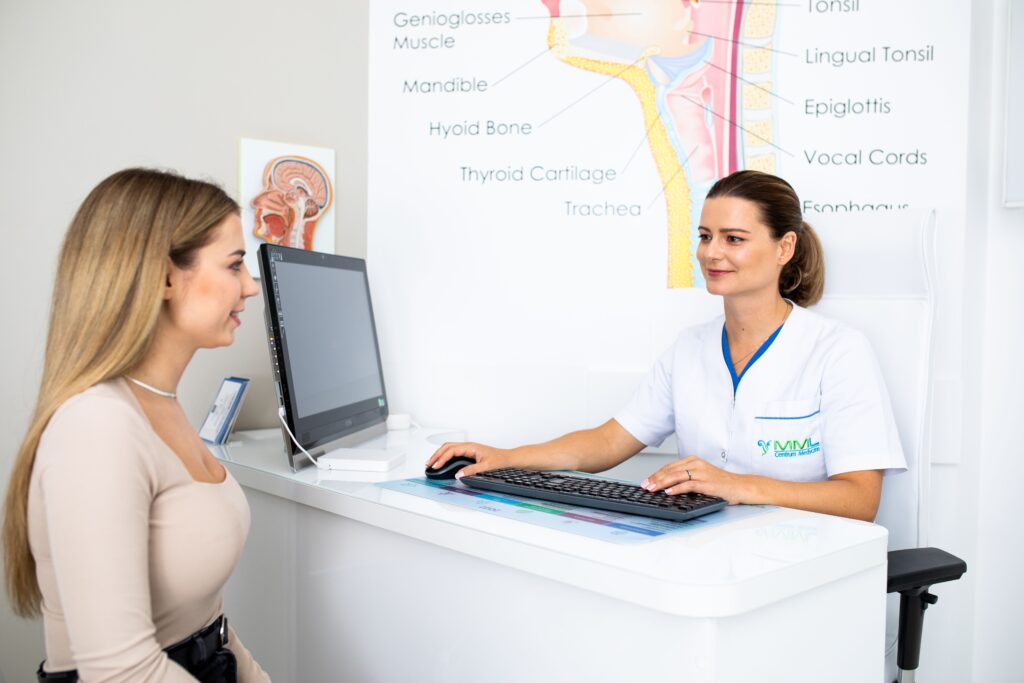
What does the test look like and what can be diagnosed during the test?
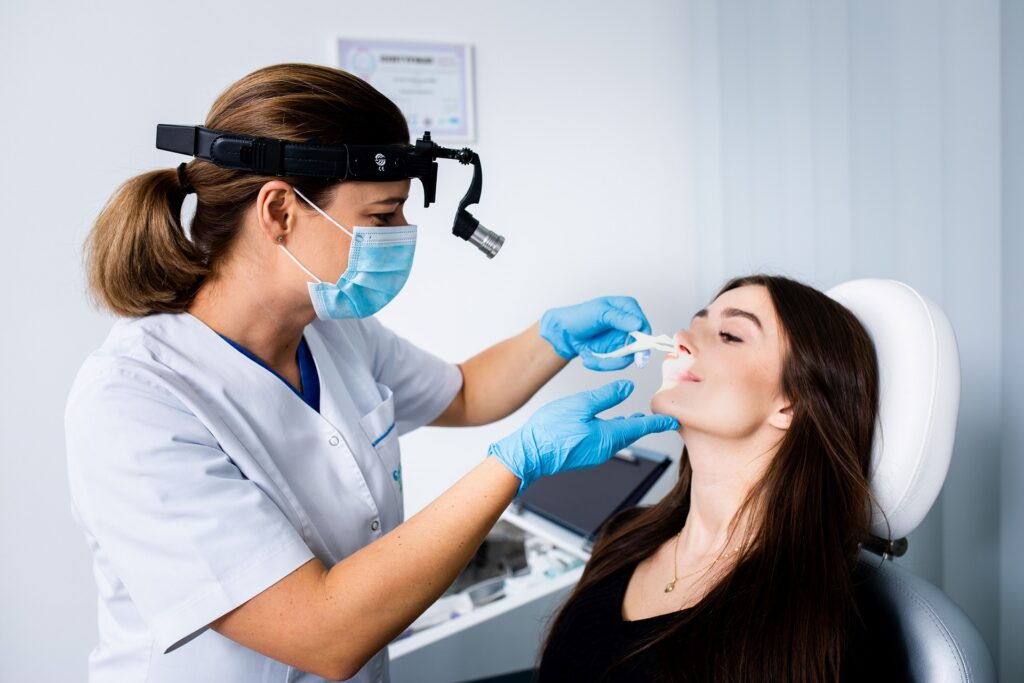
After taking medical history, the patient sits in the ENT examination chair – they can rest their head comfortably on the specially profiled headrest. The doctor uses an atomizer to administer anesthetic (lidocaine) into the nasal cavities. It looks exactly the same as when we use nasal spray.
The purpose of anesthesia is not to reduce pain (since viewing the airway with a fiberscope is painless), but to eliminate the vomiting reflex. This unpleasant sensation occurs whenever any foreign body (in this case, a fiberscope) reaches the throat.
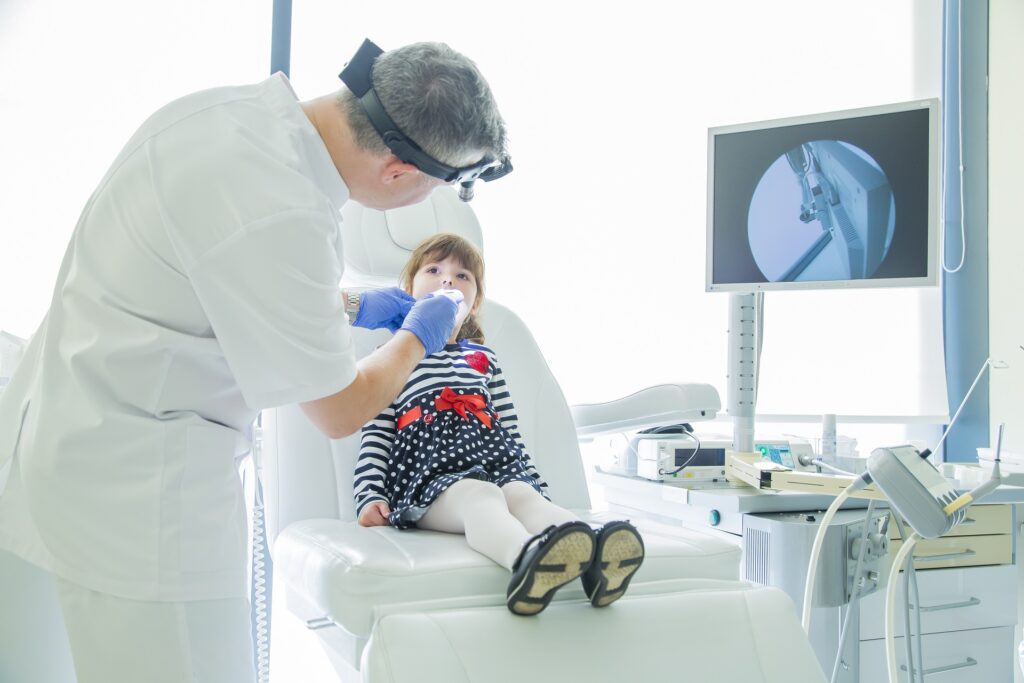
The specialist then proceeds with the examination. The specialist operates fiberscope with one hand (it is a bit like using a pad while playing Play Station) and by turning on the NBI filter from time to time observes every recess of the mucosa. The specialist explains to the patient what he/she sees on the screen. If possible, and if the patient is willing, they can view the inside of their airway themselves.